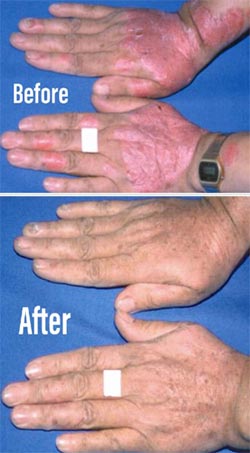
Psoriasis is a common, chronic, inflammatory, condition affecting about 2% of the population. Though it can present at any age, the usual course is diagnosis around teenage to young adulthood years with a chronic, recurring course. There is usually a family history of psoriasis, but it is important to note that in 25% of people with psoriasis, there is no known case in the extended family. While there are several sub-types of psoriasis, the most common is plaque-type psoriasis. This subtype classically appears as raised, sharply bordered plaques or small bumps with a silvery, adherent scale on top. Plaque psoriasis often affects the scalp, elbows, and knees, (although any area of the skin can be affected). The underlying cause of psoriasis is not yet fully understood. However, we do know that it is an autoimmune condition that occurs in genetically susceptible individuals. Many people recall that a stressful event had triggered their psoriasis. This is an interesting phenomenon because we know that stress may lead to changes in the immune system that may allow an underlying condition, such as psoriasis, to be expressed during the stressful event. Importantly, psoriasis is not contagious and poses no harm to those who come in contact with affected individuals.
Although there is no cure for psoriasis, the wonderful news about living with psoriasis is that there are many highly effective treatments that are now available to treat this chronic condition. With currently available therapies, most patients can maintain their skin nearly-clear and prevent symptoms of psoriatic arthritis and most importantly, halt the progression of any joint disease.
To be treated adequately, it is important that you are seen by a board-certified dermatologist for proper assessment to determine the most appropriate treatment option suitable to you.
At Skin & Beauty Center, we offer a wide range of treatment options for people living with psoriasis. Ranging from various topical agents, laser treatments with our state-of-the-art FDA-approved XTRAC excimer laser, and FDA-approved oral and injectable biologic treatments.
Our aim is for our patients with psoriasis to achieve clearance of their skin disease while minimizing side effects of their treatments. If you think you or someone you know has psoriasis, we advise scheduling a consultation with one of our board-certified dermatologists. Our providers will properly evaluate your history and perform proper skin examination to provide you with an appropriate diagnosis, counseling and management for your skin condition.