Psoriasis is a common inflammatory skin condition that affects over 7 million people in the US. Psoriasis is not contagious, so those with it do not pose a health risk to other people.
WHAT CAUSES PSORIASIS?
It is an autoimmune disease, meaning the body’s own immune system is sending out faulty signals. This causes an increase in the growth cycle of skin cells, which causes the cells to pile up and form the psoriatic lesions.
WHO GETS PSORIASIS?
There is some genetic link to psoriasis, so if you have a blood relative with the disease your chances of having psoriasis are increased. It can occur in any age, but most commonly it begins before 35.
WHAT DOES PSORIASIS LOOK LIKE?
There are multiple variations of psoriasis and sometimes more than one type can be present simultaneously.
- Plaque Psoriasis: This is the most common form of psoriasis, affecting 80-90% of those with psoriasis. You will see well defined raised red skin with white scales. It often occurs on the scalp, elbows, knees and trunk, but can be anywhere.
- Guttate Psoriasis: Small red scaly dots and patches throughout the body. It is often seen after a strep infection.
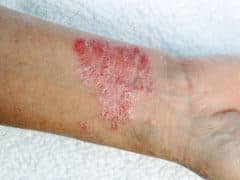
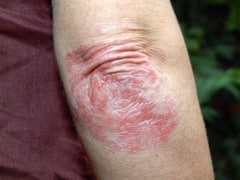
distribution on elbows.
- Inverse Psoriasis: Smooth dry patches that are found in the skin folds under the arms, in the groin and under the breasts. This is often misdiagnosed as a yeast infection, as the appearance can be very similar.
- Pustular Psoriasis: Small blisters filled with clear fluid surrounded by red skin. This is not seen often, but can be very debilitating, especially when the blisters are on the palms of the hands or soles of the feet.
- Erythrodermic Psoriasis: Extremely red skin that looks like a bad sunburn covering much of the body. Oftentimes patients are very ill with this type of psoriasis and may require hospitalization.
- Psoriatic Arthritis: Between 10-30% of psoriasis patients will develop psoriatic arthritis within 10 years of the onset of psoriasis. This causes the joints to become stiff, swollen and painful.
What Conditions Can Be Mistaken For Psoriasis?
Because the red, scaly appearance of psoriasis is similar to many other skin conditions, it’s important to get a diagnosis from an experienced dermatologist like those at any of the Skin & Beauty Center’s 7 offices.
Psoriasis is often mistaken for:
- Eczema, including seborrheic dermatitis and contact dermatitis
- Parapsoriasis
- Keratosis pilaris
- Ringworm or other fungal infections
- Pityriasis rosacea
- Lichen sclerosis
- Secondary syphilis
- Acne
- Hives
- Yeast infection
- Skin cancer
Ruling out other issues can help you get proper treatment and manage your skin condition.
Can a Child Have Psoriasis?
Psoriasis can develop at any age, from infancy to adulthood. Children are more prone to guttate psoriasis which can be triggered by common infections like strep throat. Fortunately, this type of psoriasis often disappears when the infection is cured. However, some children who have had guttate psoriasis may later develop plaque psoriasis. If your child has any rash, it’s best to seek out a diagnosis.
When deciding whether or not to treat a child with psoriasis, our dermatologists consider several factors including whether it’s causing itching and discomfort and emotional distress from the appearance of the rash. If your child is unbothered by psoriasis, their doctor might hold off on treatment and create a plan for the future instead.
Can Stress Trigger Psoriasis?
Emotional stress is one of the most common triggers for psoriasis, which makes managing mental health especially important if you have this condition. If you have psoriasis and high-stress levels, your treatment plan might include medications, talk therapy, yoga, meditation, or physical exercises to avoid this trigger. Physical stress (like having a cold or flu) is often a trigger too. Healthy lifestyle habits can help fortify your immune system against these flares.
If your psoriasis first appeared during a particularly stressful time, you might wonder if the condition is caused by anxiety. While the cause of psoriasis isn’t fully understood, it’s thought to be an immune system problem where genetics and environmental factors play a role.
Is Psoriasis Contagious?
If you have psoriasis, you don’t need to worry about passing this condition on to others. Psoriasis is not contagious and can’t be passed through skin contact or proximity. However, because some common fungal conditions like ringworm or yeast infections are mistaken for psoriasis, it’s important to rule out anything contagious.
Is Psoriasis Dangerous?
Psoriasis is more than just a scaly rash. This condition is considered a multisystem inflammatory disorder, which means you’re more likely to have comorbidities if you have it. Fortunately, except for the rare erythrodermic type, psoriasis is not considered life-threatening.
Without treatment, patients who have psoriasis are at an increased risk of several conditions. These include:
- Inflammatory arthritis: Psoriasis is associated with psoriatic arthritis, dactylitis (inflammation in the hands and feet), and enthesis (inflammation where tendons and ligaments meet bone).
- Cardiovascular disease and stroke: Because psoriasis causes long-term inflammation inside the body, it may affect the blood vessels and heart leading to a greater risk of heart attacks and strokes.
- Depression: This mental health condition is a common comorbidity of psoriasis.
Proper treatment at our Skin & Beauty Center offices can reduce your risk of developing complications or comorbid conditions.
WHAT SHOULD I EXPECT IF I HAVE PSORIASIS?
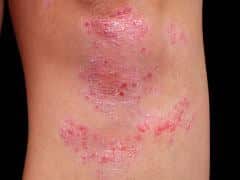
Psoriasis is a chronic, long-term disease with periods of remission and flares. You will most likely need to be on long-term medications. There is currently no cure for psoriasis, but newer medications make the long-term management of the disease much easier.
There are several trigger factors that may cause flares in your condition. The more common triggers are infections, stress, injury, hormones, smoking, alcohol, seasonal changes, and NSAIDs.
WHAT CAN I DO IF I HAVE PSORIASIS?
It is important to see your dermatologist on a regular basis, especially during times of flare. There are many treatment options available, based on the severity of your disease. These range from topical creams, solutions, gels and ointments, oral steroids, light therapy, PUVA, methotrexate, and oral immunomodulators and biologics which cause the immune system to either stop or ignore the faulty signals being sent out.
SCHEDULE YOUR CONSULTATION TODAY!
For more information on psoriasis or to schedule your skin care consultation with the Skin & Beauty Center, contact us today!
