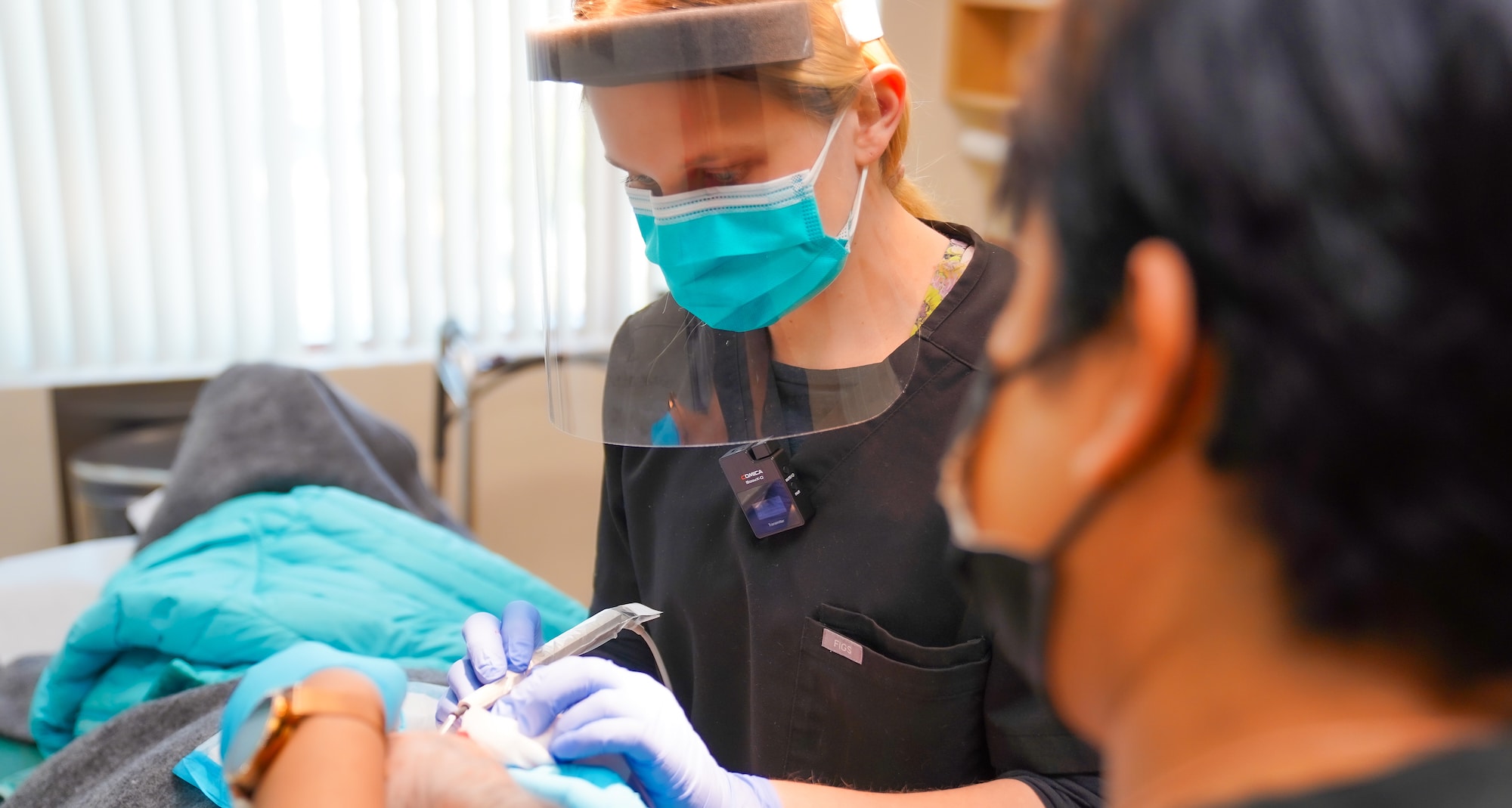
Mohs Skin Cancer Surgery at Skin & Beauty Center
Mohs Micrographic Surgery is a specialized surgical procedure used to remove skin cancers. It is a comprehensive skin cancer excision surgery used in specific circumstances. The usual indications for using Mohs Surgery to treat a skin cancer are:
- Diagnosis of an aggressive skin cancer type via biopsy
- Recurrence of a previously treated or surgically removed skin cancer
- Skin cancer that is near an important structure such as the nose, ear or eyelid
- Skin cancer in a cosmetically important area such as the face or neck
- Skin cancer that is greater than 9mm on the face or greater than 2 cm on the trunk or extremities
The procedure is done in our office under local anesthesia and can usually be accomplished in one day. Our Mohs surgeons take their time to thoroughly examine the affected area and remove any cancerous tissue while leaving healthy areas as intact as possible. This helps to reduce your risks of recurrence or spreading to other organs.
To learn more about Mohs skin cancer surgery, schedule your first consultation today.
How Does Mohs Surgery for Skin Cancer Work?
The actual technique involves several steps. First, the involved area is anesthetized with injections using a very small needle. We add a special ingredient to our anesthetic which makes the injection less painful. The local anesthesia will take 1-2 minutes to take effect, after which the rest of the procedure should involve very little discomfort.
Skin cancers tend to be softer than the surrounding skin and often the bulk of the tumor is first removed by scraping off this soft tissue. Then a thin layer of surrounding tissue is removed surgically. Next, the layer of skin that has been removed is processed and prepared for examination under the microscope by the Mohs surgeon. This tissue is carefully mapped and color-coded with dyes to enable the Mohs surgeon to determine the exact location of any residual cancer.
The processed tissue is then carefully and systematically examined under the microscope, all in-office and during the same procedure. If any residual skin cancer is found, then the entire process of tissue removal is repeated, but only for the areas where residual tumor remains.
We can usually determine if you are going to need additional tissue removed before your local anesthetic wears off. If you need additional tissue to be removed, we will give you more local anesthetic for the next stage while you are still numb from the previous injections.
The processing and microscopic examination usually takes approximately 1 hour, but may take longer if the amount of tissue removed is larger than average. It is impossible to determine ahead of time how many times this process will need to be repeated.
Have additional questions? Give us a call now at (818) 842-8000.
How Should I Prepare for My Mohs Micrographic Surgery?
We ask that you come to the office 30 minutes prior to your appointment time and expect to stay up to 6 hours, but it does not always take that long. Take your medications, if any, as usual, including aspirin or any other blood thinners you may be prescribed.
We encourage you to bring a book and/or media player with headphones with you to help pass the time. We also require that you arrange for someone to drive you home. If you so desire, your accompanying friend or family member can wait with you during the time you are in the office. After the skin cancer has been removed, we will determine how to treat the excision area.
In some cases, the excision wound can be allowed to heal by itself, which may take several weeks or months depending on the size of the wound. Sometimes the wound can be closed directly with stitches if the wound is not too large. If the excision area is larger, then some of the surrounding skin may be used to cover the wound (this is called a flap) and then the area closed with stitches.
In some cases, a skin graft may be required to help cover and heal the affected area. We will decide together what will be best for you after all the skin cancer has been removed.
What Should I Do for Post-Surgery Care and Recovery?
You will be given written instructions after the surgery on how to care for the treated area. Frequent bandage changes will be necessary, as the wound will drain during the healing process. Most bandages should be changed at least once a day. Mild bleeding can also occur following this type of surgery. If bleeding should happen, apply direct, constant pressure without stopping for 20 minutes. If the area is still bleeding after pressure then call the office, even if it is after regular office hours.
You can expect some mild discomfort after the anesthetic wears off. Usually plain Tylenol is sufficient to control the pain. Swelling and bruising are quite common after this type of surgery and should resolve in 2-3 weeks. Skin cancers can often involve the nerves of the skin and it may take as long as a year or two until normal sensation returns. It is possible that the area may stay numb permanently.
The treated skin area can often feel tight. This tightness improves after several weeks to months. Skin cancer removal surgery will result in scarring. We will try to give you the best cosmetic result possible; however, the most important aspect is removing the entire tumor with the highest chance of it not recurring. Fortunately, scars tend to improve with time, but the maximum improvement may take as long as 1-2 years.
Rest assured we will always be available to you should you have any questions or develop problems.
Call (818) 842-8000 or schedule your appointment online today to learn more about Mohs micrographic skin cancer surgery and other skin cancer treatment options at Skin & Beauty Center.
