Skin cancer is the most common form of cancer. In the US alone there over 5.4 million cases of non-melanoma skin cancer (basal cell carcinoma and squamous cell carcinoma) treated each year in over 3.3 million people.
As Americans are living longer it is now estimated that 1 in 5 of them will be diagnosed with some form of skin cancer in their lifetime. These non-melanoma skin cancers are not usually aggressive and very rarely metastasize.
Most patients affected with these types of skin cancer are able to lead normal, healthy lives if diagnosed and treated early. When left unattended, however, these skin cancers can cause significant localized symptoms such as bleeding and pain. They may become locally destructive to underlying and nearby structures causing disfigurement and disruption of function of vital structures such as the eyes, nose and ears.
When Should I Get a Skin Cancer Exam?
Most people may not be able to detect non-melanoma skin cancers as they usually do not have the classic worrisome signs of skin cancer.
Everyone should get full skin exam by a dermatologist on annual basis. This is especially important in those individuals who have risk factors for developing non-melanoma skin cancers. These risk factors include:
- excess exposure to UV radiation from the sun
- fair complexion
- tanning bed use and frequent outdoor tanning
- suppressed or weakened immune system
- pre-cancerous skin lesions and prior skin cancer history
What Happens During a Skin Cancer Exam?
During a skin cancer screening, your dermatologist will thoroughly examine your skin, including common areas where skin cancer may form such as the face, neck, arms, and legs. They may also offer specific recommendations tailored to your lifestyle and risk factors.
It's important to perform monthly self-exams between your annual skin exams to aid in early detection. Non-melanoma skin cancers come in variety of colors and textures. Lesions that slowly enlarge over time, bleed easily or fail to heal as expected over a few weeks should raise suspicion and thus should be evaluated by a dermatologist as soon as possible.
The “ABCDE” criteria below were developed in order to help patients detect suspicious moles during self skin examinations:
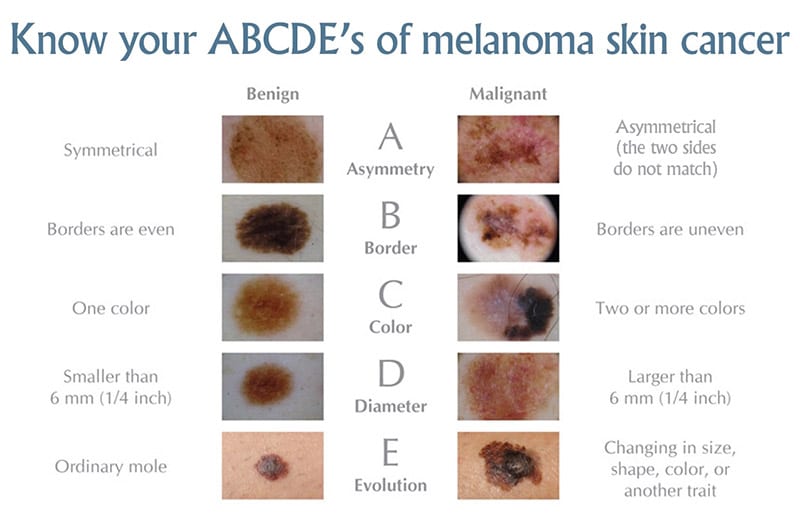
A mole that meets any of these criteria is not necessarily cancerous but rather that it should be clinically evaluated by a dermatologist. Of the above criteria the most important to keep mind is “evolution”: any rapidly changing mole or any “ugly duckling” mole (i.e. mole that appears different than rest of one’s moles) should be evaluated by a dermatologist. Furthermore, any newly appearing moles, especially in patients over 30 years of age, require clinical evaluation.
What is the Most Dangerous Skin Cancer?
The other major category of skin cancer is malignant melanoma which, while only accounting for less than 1% of all skin cancers, accounts for majority of deaths from skin cancer.
This is because, unlike basal cell and squamous cell carcinomas, melanomas behave aggressively and can become metastatic (i.e. spread to other distant sites of the body) if left untreated. Therefore, early detection and treatment of melanomas is of utmost importance in determining survival.
Less than half of melanomas arise from pre-existing moles and that majority of melanomas are flat and not raised.
How Do I Prevent Skin Cancer?
Protection from UV radiation from the sun and avoiding artificial tanning are the most effective ways in reducing one’s risk factor for skin cancers.
Sunscreens with an SPF (sun-protection factor) rating of 30 or higher should be applied to all sun exposed sites on a daily basis and then reapplied every 90 minutes if out in the sun. This is especially important during the peak UV radiation hours of 10 AM to 4PM. When possible, seek shade and wear a hat when out in direct sunlight.
Be sure to practice these measures on routine basis and stay vigilant of suspicious skin lesions with monthly self skin exams. Just as important is visiting your dermatologist at least once a year for skin screening. In combination these measures will result in earlier detection and treatment of skin cancers and thus allow one to lead a normal, healthy life even when a skin cancer diagnosis is made.
